MedTrainer’s provider enrollment and credentialing services and best-in-class credentialing management software accelerate document collection, verification, enrollment applications, and payer follow-up. Finally insurance credentialing services you can rely on!
Discover how MedTrainer can help you get credentialing done right, every time.





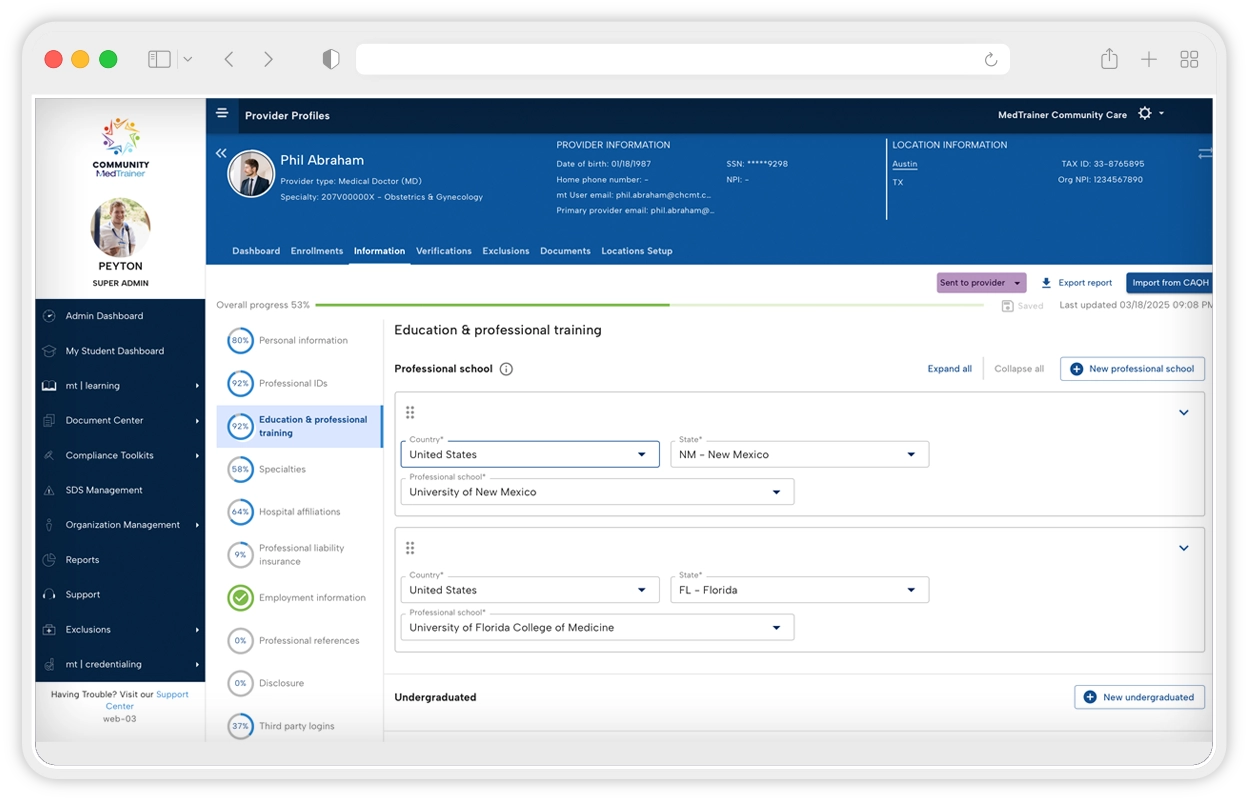
Work smarter, not harder with a proven platform built by experts and enhanced with artificial intelligence (AI). MedTrainer’s provider enrollment software speeds up data collection with a full-access CAQH integration and bulk document upload with AI-powered classification.
Improve the speed and accuracy of enrollment applications with automatic form fill and credentialing packet generation. Plus, easily enroll multiple providers at the same time with group enrollments.

MedTrainer’s experienced, in-house team executes your credentialing from end-to-end, including provider enrollment and getting credentialed with Medicare.
Our insurance credentialing services go far beyond just application completion — data management, linkages, accurate submission, follow-up with payers, and management of re-submission is all included.
If you’re struggling with managing credentialing on your own, are unsure how to get credentialed with insurance, or are just looking to outsource, we’ve got you!
Credentialing software is the most effective way to reduce delays and fast-track revenue generation. Even cutting just a few days from your current insurance credentialing timeline can result in thousands of dollars in revenue.
Rely on MedTrainer’s medical insurance credentialing services — our platform is the Most Implementable according to G2’s Summer 2025 Reports, and is consistently ranked as a Momentum Leader for its rapid innovation.
